Ticks perch on top of grass, brush, trees and other shrubs waiting for a host to walk by. They cannot jump and are completely blind, but can sense warmth and smell the butyric acid emitted by warm blooded creatures from several yards away. When they hone in on their target, they drop from their perch onto the perspective host.
The list of tick-borne illnesses that can affect dogs is as long as the names are difficult to pronounce
By Casey Sill
Ticks have the rare and precarious ability to give even the heartiest outdoorsmen and women a bone-cracking bout of the hibbie jibbies.
Last summer I watched two of my close friends, both of whom spent six years in the infantry in some of the toughest conditions on the planet, lose their cool over ticks on a camping trip in southern Iowa. I basked in the glow of silent judgment at the time.
I’d always been pretty nonchalant about ticks and the threats they carry, so a heavy dose of smugness arose as I watched their skin crawl all weekend with both real and imaginary bugs. But a couple months after that camping trip my English setter Loxley couldn’t get up one morning and later tested positive for both Lyme and Anaplasma. She was fine of course after the normal series of antibiotics, but seeing how sick she was has made me take ticks a little more seriously in the time since.
As winter officially begins to give way to spring and we edge closer to the start of training season across much of the country, it’s an important time to brush up on our knowledge of tick borne illness, as well as tick prevention tactics.
What’s out there
The list of tick-borne illnesses that can affect dogs is as long as the names are difficult to pronounce, but there’s a handful that deserve most of our attention. Lyme disease is the leader in both familiarity and frequency, but Anaplasma, Ehrlichiosis and Rocky Mountain Spotted Fever are also very common in the US — increasingly so in recent years. Here’s a breakdown of those four illnesses.
Lyme Disease
Lyme Disease is the most common vector-borne illness in the United States. It’s an infectious disease caused by a spirochete bacteria Borrelia carried by the Black-Legged Tick, more commonly known as the Deer Tick. Lyme disease has typically been associated in the northeast and upper Midwest, but it’s now also being seen on the west coast and in Florida.
Symptoms of Lyme disease may include fever, lameness, limping, joint pain/swelling, enlargement of lymph nodes and lethargy. Untreated Lyme disease can progress to kidney disease, which can be fatal.
Anaplasma
Anaplasma is carried by the Black-Legged Tick. Though Anaplasma can be seen worldwide, there are two Anaplasma species that are known to detect disease in North American dogs.“Phagocytophilum” in the Northeast and the upper Midwestern United States and “Platys” in California and coastal states. The symptoms of Anaplasma are similar to Lyme disease, though dogs often also have low blood platelets, which can cause bleeding disorders.
Canine Ehrlichiosis
Canine Ehrlichiosis is found worldwide, and is caused by several types of ticks — The Brown Dog Tick, Lone Star Tick and American Dog Tick. Signs include fever, poor appetite and low blood platelets, often noted by nose bleeding or other signs of bruising or anemia. Signs start about one to three weeks after the bite of an infected tick. Dogs diagnosed and treated promptly can have a good prognosis, but those who go on to the chronic phase have more difficulty recovering.
Rocky Mountain Spotted Fever
Rocky Mountain spotted fever is one of the more commonly known tick-borne diseases to affect both dogs and humans. It’s carried by the American Dog Tick and the Rocky Mountain Wood Tick, as well as the Brown Deer Tick. This disease has been found in much of North, South and Central America. The symptoms once again mimic those of Lyme disease, and include — fever, poor appetite, swollen lymph nodes and joint pain. Low platelets, which help in blood clotting, are often found. On occasion, neurological issues can also occur.
Expanding threats
Climate shifts and loss of habitat affects parasitic bugs just as much as it does migratory and upland birds. The geographical range for all of these diseases is changing, and hunting dogs are particularly susceptible to these changes.
Dr. Jennell Appel is a veterinarian based in southern Georgia. She runs a mobile vet care unit at national field trials all over the country and sees the full spectrum of tick borne diseases on a regular basis.
“The changes have a lot to do with the migration patterns of birds and deer,” she said. “We call them vectors — animals that hold on to the diseases and take them other places. As their patterns and ranges shift, so too do the ticks.”
The issue is compounded further in the working dog world, since the dogs themselves are also vectors.
“I used to tell people in certain areas not to worry too much about ticks and tick prevention, but not anymore,” Appel said. “Because even if ticks aren’t as prevalent in a certain area, what we don’t think about are dogs coming into that area with disease. We constantly have dogs moving all over the country. So even if a disease isn’t in your area, it can be brought in very easily.”
Prevention
Dr. Appel now recommends year-round tick prevention for bird dog owners, regardless of your geographic location. There are a number of affective treatments on the market, but she warns against any topical tick prevention for sporting dog owners.
“I do not recommend any topicals for field dogs, whatsoever,” she said. “Our dogs are in the water way too much, and I don’t care what the box tells you, when your dog is in water consistently, you’re losing the efficacy of that product.”
Simparica Trio and NexGuard are the two treatments Dr. Appel recommends today. Both have been through extensive clinical trials and have stood the test of time. Dr. Appel said steer clear of any shiny new products that aren’t yet proven.
“People want to jump on the bandwagon, but I never recommend anything until it’s been out there for a while,” she said. “There’s been a lot of products come out and a year later we’re having all sorts of side effects. Simparica Trio and NexGuard have been really safe and I’ve had zero issues with them.”
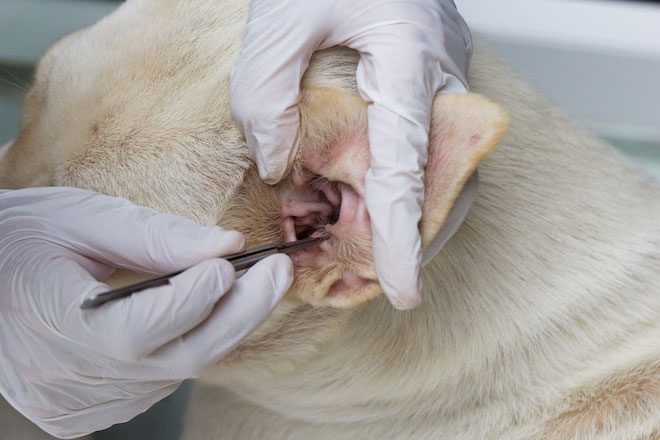 Dr. Appel recommends any long-nosed instrument for tick removal. Surgical hemostats and tweezers both work well. She said it’s important to never use your hands to remove a tick, since disease can be spread from the tick to bare skin during removal.
Dr. Appel recommends any long-nosed instrument for tick removal. Surgical hemostats and tweezers both work well. She said it’s important to never use your hands to remove a tick, since disease can be spread from the tick to bare skin during removal.
Even with the regular use of tick prevention products, once in a while one will slip through and bite a dog. For removal, Dr. Appel recommends anything with a long, skinny tip. A surgical hemostat works best, but needle nose pliers will do in a pitch. There are also several solid tick removal products on the market like the “Tick Twister.” Dr. Appel also said no matter what instrument you use, it’s important to have your own safety in mind when removing ticks.
“It’s important to remind people that we know scientifically there can be transmission between a tick and a human when we’re removing a tick,” she said. “I’m guilty of forgetting that as well, but we need to be very careful.”
What does Lyme look like?
Lyme disease on a layman’s level is most commonly associated with stiffness and joint pain. This can come and go to different parts of the body, something Dr. Appel calls “shifting lameness.” It’s her number one identifier that a dog may have Lyme, and it’s not always overly obvious.
“Most often they’ll just be intermittently stiff. One day the dog might be stiff on their right front, and the next day its their left hind,” she said. “Whenever an owner tells me their dog kind of seems lame all over, that’s when my red flag goes up.”
One of the reasons Lyme is such a moving target is these symptoms can take months to occur after infection, or may not ever surface physically.
“It’s really all over the map. It ranges from a dog that develops acute symptoms within 48 hours of a tick bite to a dog that has literally no clinical signs,” she said. “I’ve diagnosed some dogs based on an X-ray that shows joint damage years after infection.”
Treatment
Dr. Appel’s standard treatment for tick borne illness is an eight week course of the antibiotic Doxycycline, but there’s a misconception among many people that after those antibiotics have run their course the disease is no longer present in the body.
“You can never actually clear Lyme from the body, once a dog has it, they’ll always have it,” she said. “So I will retest a dog six months later and look for antibody levels, and again a year after that. If those numbers start to creep up, I’ll treat the dog again.”
Part of the reason for the constant stream of new preventative products on the market is ticks themselves are also changing. They’re becoming resistant to some of the chemical compounds in these products, as well as slowly developing resistance to the drugs used in treatment, which could render them less effective over time.
“There’s going to come a point where doxycycline is not going to work with every disease,” she said. “So looking forward, I put a heavy priority on funding studies on tick borne diseases.”
Recent studies have revealed different strains of Lyme and other diseases, as well as new information about the timing of transmission. Until recently it was widely believed in the veterinary community that ticks could not transmit Lyme or other diseases until they’d been attached for 48 hours, but new research changed that standard to under 24 hours. It’s progress like this that will help Dr. Appel and other veterinarians adapt to the changing face of tick borne illness.
“Our dogs are exposed to these diseases on a daily basis, and it’s not going away,” she said. “So the fact that the diseases are changing, the ticks are becoming more resistant, that’s going to be a continual problem.”
It’s important to remember almost all these lessons apply to us as well. Lyme is as pervasive in humans as it is in canines, and the number of cases per year has increased dramatically in the last decade or so. On top of that, we also have to watch out for Alpha-gal syndrome, the red meat allergy caused by the bite of a lone star tick.
Most of the ticks we spent time with on that camping trip in Iowa were lone star ticks. After we got home my buddies were texting back and forth in a group chat about Alpha-gal. Symptoms, long term effects, etc. — I continued my ribbing.
“Oh, we’ll be fine you big chickens.”
Couple nights later I pulled one of them out of my left arm pit that looked like it’d been attached for a while. I spent the next 45 minutes frantically scrolling back through the texts, slowly convincing myself I’d never be able to eat beef again.
The panic was brief but real, and I never admitted my hypocrisy to either of my friends. But between that and Loxley’s bout with Lyme, I’ll certainly be a little more cognizant as I head out into the field to train dogs and hunt turkeys this spring.
Casey Sill is the public relations specialist at the Pheasants Forever national headquarters in St. Paul, Minn. He can be reached at csill@pheasantsforever.org.